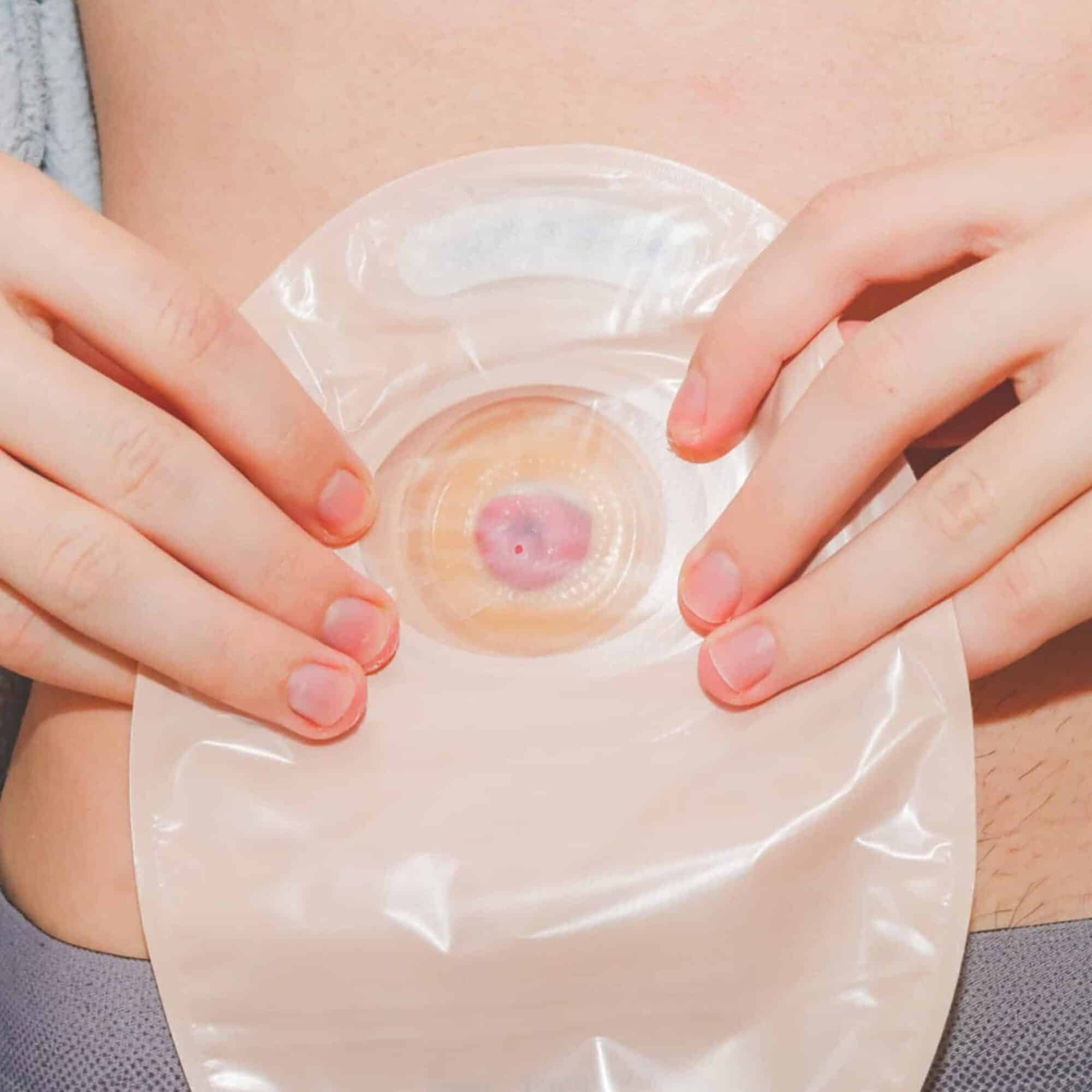

Family Nursing & Home Care (FNHC) have experienced professionals who work with patients who have a stoma. There are many reasons why a patient may need a stoma, which can be temporary or permanent. A stoma involves an opening in the abdomen which is connected to the digestive or urinary system in order to allow waste to be safely diverted from a patient’s system.
At FNHC we understand how life changing a stoma operation can be and our expert nurses work with our patients to show them how to clean their stomas and how to change stoma bags. They also give advice on how patients can manage their stoma at home, making them aware of the different options available, with dignity at the core of our service.
Contact Us
Get in touch about our services
You can contact the District Nursing Team on (01534) 497600 or complete the short form and we will get back to you.
"*" indicates required fields
News & Stories

FNHC signs up to Rainbow Mark Programme
By Family Nursing & Home Care
Thursday 26 June 2025
FNHC delighted to receive grant from the Parish of St Saviour
By Family Nursing & Home Care
Thursday 19 June 2025
FNHC celebrates another successful Colour Festival fundraiser
By Family Nursing & Home Care
Wednesday 30 April 2025
FNHC publishes its 2024 Impact Report
By Family Nursing & Home Care
Tuesday 15 April 2025
A new website location for Child Accident Prevention Jersey
By Family Nursing & Home Care
Wednesday 05 March 2025



